Transformational Breast Cancer MDT Support Tool
Dramatically Faster Breast Cancer Recurrence Risk Quantification

What is the Digistain Test?
Digistain is an MHRA-cleared, UKCA-marked AI-enabled quantitative histopathology platform designed to assess the risk of recurrence in breast cancer patients following surgery. It provides risk stratification information to support MDT discussion; not intended to replace clinical judgement.
The test generates a clear, easy-to-interpret risk stratification output. By providing clinicians with crucial insights, Digistain supports the development of personalised treatment plans, ensuring patients receive the best possible care while avoiding unnecessary chemotherapy.
Digistain is for invasive breast cancer patients who are:
Stage I - II
HER2-
ER+
up to 3 positive lymph nodes
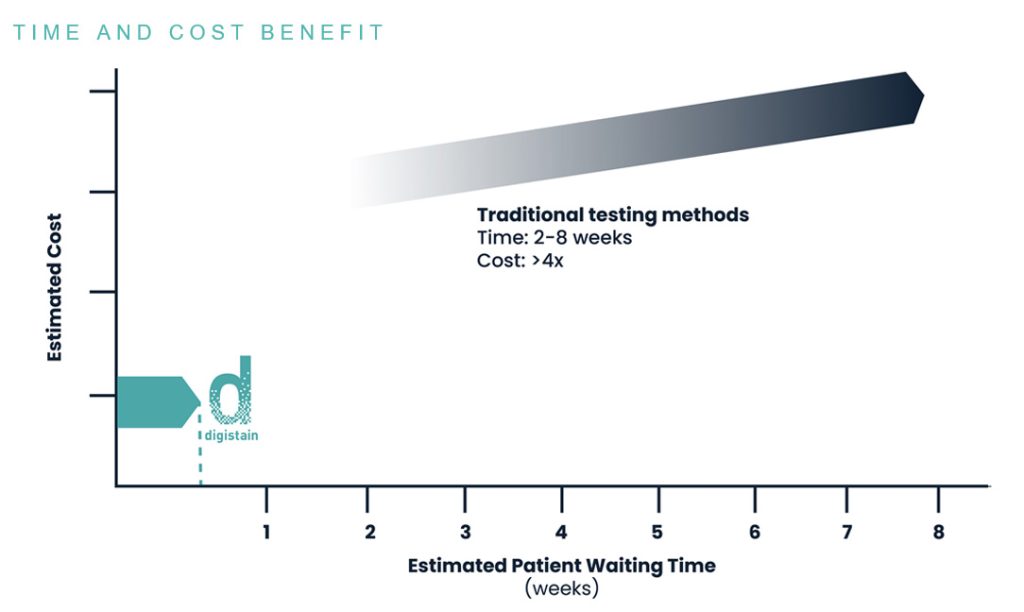
Why Digistain?
Traditional methods of breast cancer risk stratification are slow and expensive, using costly reagents and taking 2-8 weeks to deliver results.
Digistain operates on routine FFPE tissue sections, requiring no molecular extraction and integrating seamlessly into existing histopathology workflows — delivering actionable results at a fraction of the cost and time of conventional methods.
Key Benefits:
CLEAR insights on likelihood of breast cancer recurrence within the next 10 years
FAST actionable results helping reduce treatment decision times
LOWER COST enables many more people to access cancer recurrence prediction tests
SEAMLESS integration with existing clinical workflows